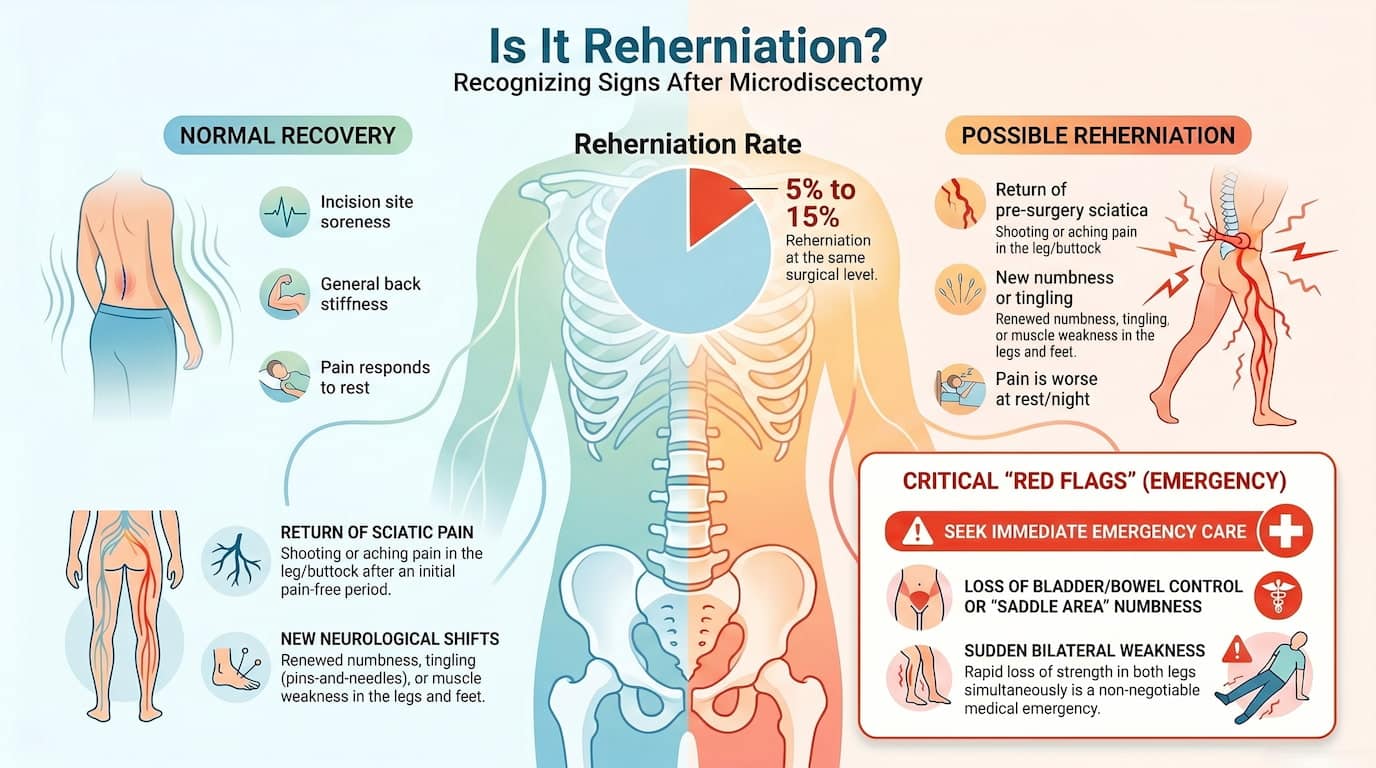
Microdiscectomy is one of the most common and successful spine surgeries, with most patients experiencing significant relief from leg pain and nerve symptoms. However, for a small percentage of patients (roughly 5 to 15%), the disc can herniate again at the same level. Knowing what to look for can make a real difference in how quickly you get the right care.
Medical Disclaimer
The information in this article is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. If you are experiencing symptoms after microdiscectomy, always consult a qualified healthcare provider before making any decisions about your care. The team at Capilano Physiotherapy Clinic offers free consultations. Reach out if you have concerns about your recovery.
1. Pain Signals: When Discomfort Comes Back
The most recognizable sign of reherniation is the return of pain that had previously improved or resolved after surgery.
Return of leg pain (sciatica). After microdiscectomy, sciatic pain typically fades within weeks. If that familiar shooting or aching pain down your leg, buttock, or calf returns, especially after a pain-free or improved period, it is the most common indicator of reherniation.
Pain that radiates from the lower back into the leg. A dull or sharp pain that travels along the same nerve path as before surgery deserves attention. This radicular pattern follows the compressed nerve’s distribution and tends to be worse in specific positions.
Increased pain at rest or at night. Normal post-surgical discomfort generally improves with rest. If your pain is worsening when lying down or waking you at night, this is not typical recovery and warrants evaluation by a musculoskeletal physiotherapist or your surgeon.
2. Neurological Signals: Changes in Sensation and Strength
Reherniation can compress the nerve again, leading to neurological changes that go beyond pain.
Numbness or tingling in the leg, foot, or toes. Renewed pins-and-needles sensations, particularly if they match the distribution you experienced before surgery, suggest the nerve is being irritated again.
Muscle weakness. Difficulty lifting your foot (foot drop), weakness when going up stairs, or reduced grip strength in your calf or thigh muscles can indicate nerve compression returning. This type of symptom warrants prompt assessment.
Changes in reflexes. A loss or reduction in the knee or ankle jerk reflex (something your physiotherapist or doctor can test) can be an objective indicator that nerve function has been affected again.
If you notice any of these neurological changes, a structured assessment through lumbar disc herniation rehabilitation can help determine the severity and guide your next steps.
3. Red Flags: Seek Immediate Medical Attention
Some symptoms require urgent care and should never be ignored or managed at home.
Loss of bladder or bowel control. This is the most serious warning sign and may indicate Cauda Equina Syndrome, a rare but serious compression of the spinal nerve roots. If you experience difficulty urinating, incontinence, or loss of sensation in the inner thighs and groin (“saddle area”), go to the emergency department immediately.
Sudden severe weakness in both legs. A rapid and significant loss of strength in both lower limbs simultaneously is a red flag that needs emergency evaluation.
These red flags are rare, but they are non-negotiable. Do not wait for a scheduled appointment if you experience them.
4. Reherniation vs. Normal Recovery Pain: How to Tell the Difference
Not every ache after microdiscectomy means something has gone wrong. Understanding the distinction helps reduce unnecessary anxiety.
| Normal Recovery | Possible Reherniation |
|---|---|
| Soreness around the incision site | Return of pre-surgery leg pain or sciatica |
| General stiffness in the lower back | New or returning numbness/tingling |
| Fatigue and muscle achiness | Weakness in legs or feet |
| Gradual, steady improvement | Improvement followed by sudden worsening |
| Pain that responds well to rest | Pain that is worse at rest or at night |
The key question is: did your symptoms improve after surgery and then get worse again? If yes, that pattern is more consistent with reherniation than with normal healing.
5. When to See a Physiotherapist
You do not always need to go straight to your surgeon. A physiotherapist who specializes in spinal conditions can assess your symptoms, determine whether they are consistent with reherniation or another cause, and build a targeted recovery plan.
Early physiotherapy after surgery, even before any concerns arise, is one of the best ways to protect the disc, strengthen the muscles around the spine, and reduce the risk of reherniation. Back pain treatment guided by an experienced clinician focuses on the movement patterns and loading strategies that reduce stress on the healing disc.
At Capilano Physiotherapy Clinic in North Vancouver, we offer free consultations for people who are unsure whether their symptoms need attention. Our team has experience in post-surgical spine rehabilitation and can help you understand what you are experiencing and what to do next.
Book a free consultation or call us at (778) 743-6090. We are open seven days a week.
Summary
Reherniation after microdiscectomy is not common, but it does happen. The main signs fall into three clear categories: the return of pain (especially sciatica), new or returning neurological symptoms (numbness, tingling, weakness), and in rare cases, serious red flags like loss of bladder control that require emergency care.
If something feels off after your surgery, trust that instinct. Early assessment almost always leads to better outcomes than waiting.